Sleep Apnea
& Snoring
Loud snoring is not always “harmless.” If accompanied by breathing pauses, gasping or coughing during sleep, or excessive daytime sleepiness, it may indicate Obstructive Sleep Apnea (OSA). Proper diagnosis is achieved through targeted clinical evaluation and a sleep study, with treatment tailored specifically to your needs.
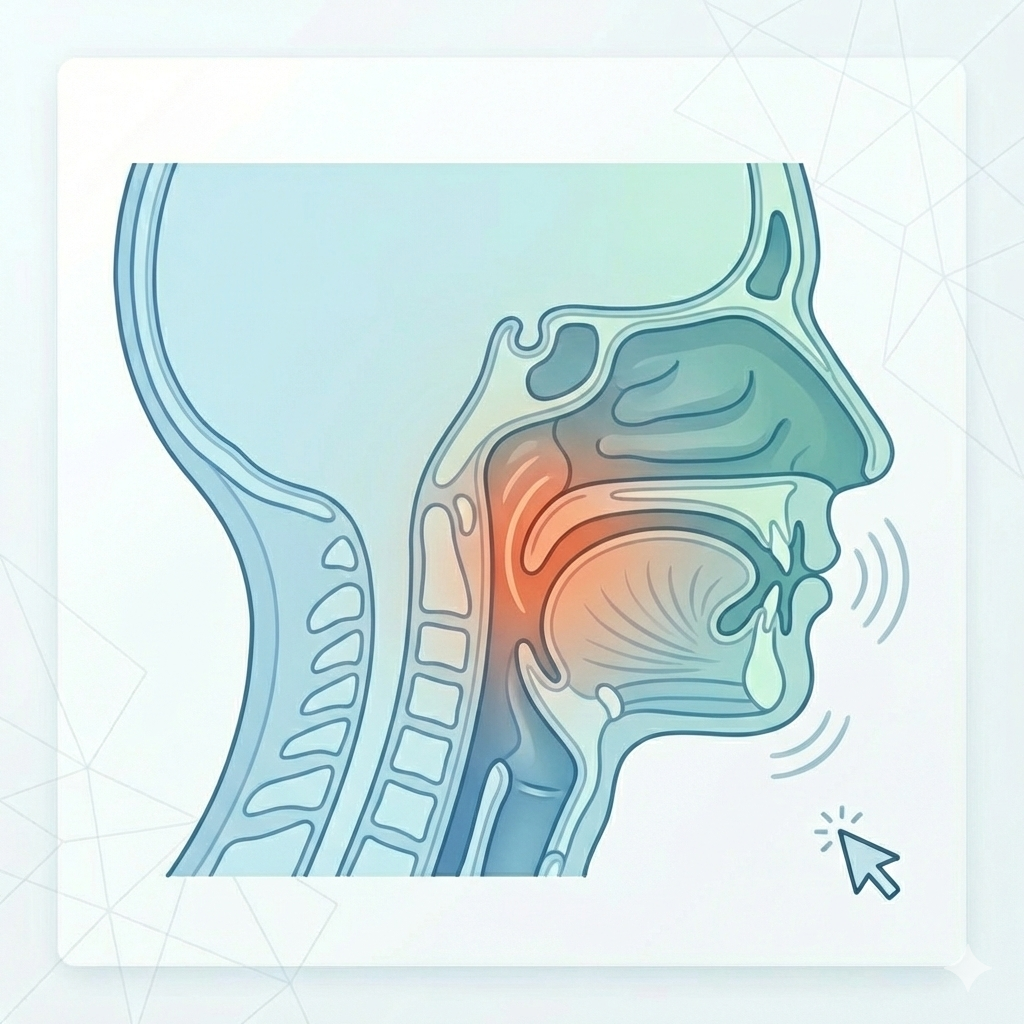
What is Snoring?
The sound caused by vibrations of soft tissues (soft palate/uvula, tongue, lateral pharyngeal walls) due to the narrowing of the airway during sleep.
Repeated episodes of partial or complete upper airway obstruction during sleep, which can lead to drops in oxygen levels and micro-arousals.
Causes
What are the symptoms?
Loud, daily snoring (especially in the supine position)
Breathing pauses observed by a partner during sleep
Choking/gasping and restless sleep throughout the night
Morning headache, dry mouth, and “brain fog”
Frequent nighttime urination (nocturia)
Daytime sleepiness and impaired concentration/memory
Irritability and decreased libido
Hypertension (especially hard-to-regulate blood pressure)
Diagnosis & Treatment Path
What do we do at the clinic?
The diagnostic approach is personalized and includes:
- 1. Medical History: Evaluation of sleepiness and sleep quality.
- 2. ENT Examination: Endoscopy of the nose, pharynx, and larynx.
- 3. Risk Factors: Assessment of weight and blood pressure.
- 4. Sleep Study: Home testing or polysomnography.
- 5. DISE: Drug-Induced Sleep Endoscopy for obstruction site.
When is treatment required?
Intervention is considered necessary when:
- Evidence of apnea / hypopnea (or strong suspicion).
- When daily snoring impacts quality of life or relationships.
- Presence of daytime fatigue or comorbidities like hypertension.
- When significant oxygen desaturations are observed.
How is it treated?
1. Lifestyle Changes
- Weight loss (critical contribution)
- Avoiding alcohol before sleep
- Position Therapy (side sleeping)
- Breathing regulation (rinses/sprays)
2. Mechanical Support
- CPAP: The “gold standard” for apnea
- Oral Appliances (MAD): Advancement devices
3. Nasal Obstruction Therapy
Improves snoring and CPAP tolerance through septum and turbinate correction.
4. Targeted Surgery
Based on DISE mapping:
- Uvulopalatopharyngoplasty (UPPP)
- Tonsillectomy / Tonsillotomy
- Tongue base & hypopharynx interventions
GOAL: Opening the airway where it actually narrows.
Better & deeper sleep
Reduced snoring & a quieter partner
Reduction in sleepiness and fatigue
Improved blood pressure & cardiovascular health
ENT Clinic – 16 Kapetan Chrona St., Neo Psychiko
contact@festas-orl.gr
16 Kapetan Chrona St.

